HPTA Restart Protocol for Discontinuing TRT (2021)

Symptoms Can Return When You Discontinue TRT
If you’re thinking about stopping TRT, there is a protocol that can help prevent hormone withdrawal symptoms by restoring your own hormone production.
When you stop receiving exogenous Testosterone (Testosterone from outside the body), your deficiency symptoms will likely return.
Also, it’s possible that your testes have gone dormant, which means they need to be restarted so they can produce Testosterone again.
You may experience:
- Depression, anxiety, and other mood changes
- Erectile dysfunction and loss of libido
- Fat gain
- Changes in sleep patterns and insomnia
- Loss of strength, muscle mass, and energy
What is the HPTA Axis, and What Does it Mean to Restart It?
Men who have been taking testosterone or similar androgens for a long period of time (more than four weeks) may experience secondary hypogonadism produced by the negative feedback response to the testosterone supplementation.
This results in the body slowing down or stopping its own production of testosterone.
Sometimes the body does not recover quickly enough on its own, leading to a reduced quality of life and symptoms related to low testosterone.
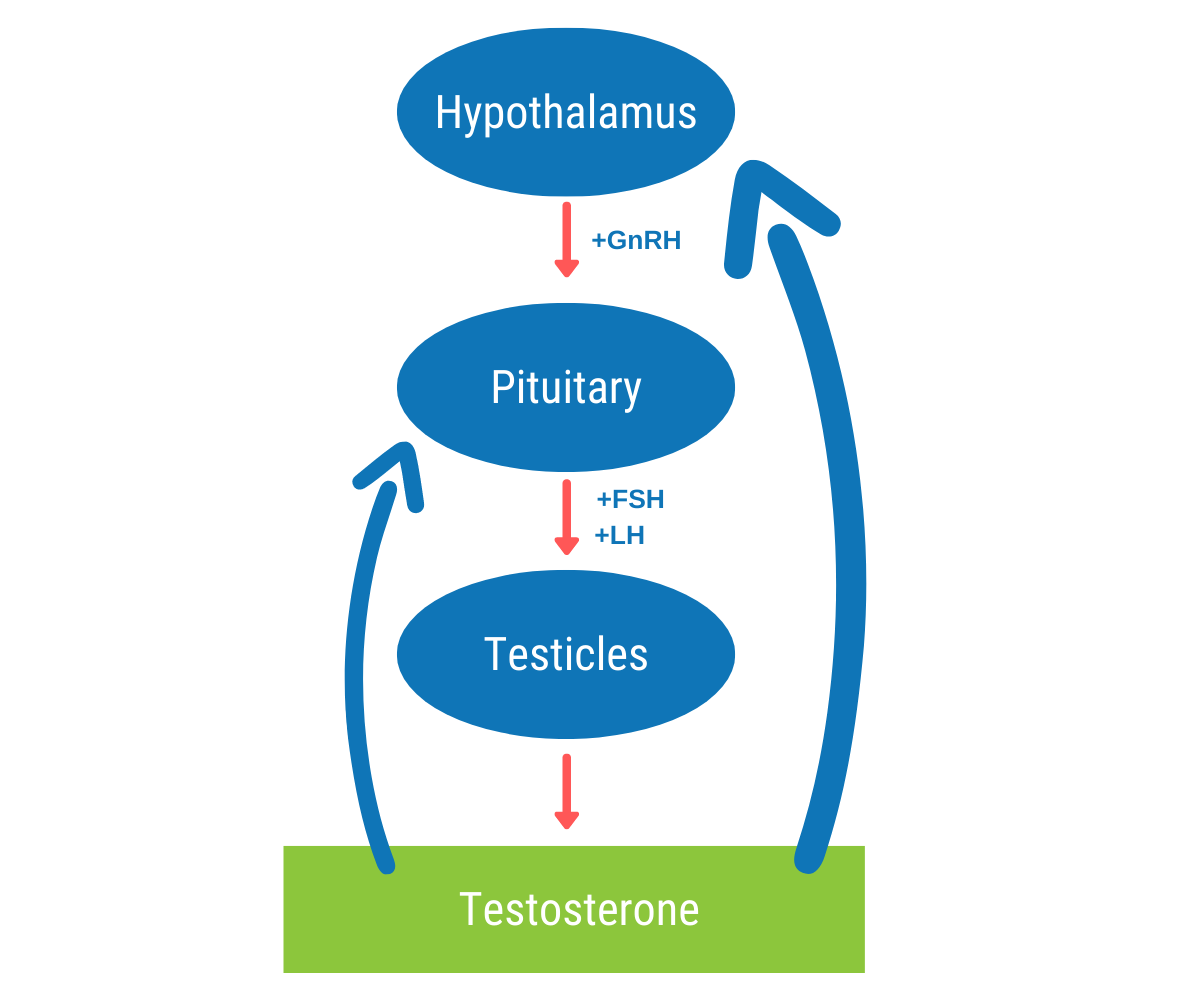
Natural testosterone production relies on a balance of hypothalamus hormones including gonadotropin releasing hormone (GnRH), pituitary hormones including luteinizing hormone (LH), and the testicles where testosterone is produced. This is called the Hypothalamus-Pituitary-Testicular axis, or HPTA.
When the body recognizes elevated hormones in the blood, it prevents the pituitary from releasing LH, and without stimulation from LH, the testicles are unable to produce testosterone.
This is not a problem in men who are supplementing testosterone (TRT), but once the hormone is discontinued, there is nothing to replace it. The result is hormone withdrawal symptoms.
HPTA Restart Protocol for Men Discontinuing TRT
Most common protocols used to restart natural testosterone production utilize a combination of hormone stimulators designed to address the different areas affected by negative feedback.
This includes the stimulation of LH production in the pituitary or stimulation of the testicular cells to produce testosterone.
Sometimes, a combination protocol is prescribed to first increase testicular volume and testosterone production using a gonadotropin like HCG, followed by pituitary stimulation to increase LH production using a class of medications known as selective estrogen receptor modulators (SERMS). Since HCG mimics LH, the goal is for the body’s LH to take over communicating with the testicles to maintain volume and adequate testosterone production.
There may be cases where a patient cannot maintain adequate testosterone production on their own after discontinuing hormone supplementation. The HPTA restart protocols can also be used as a diagnostic tool to help the physician determine where the body is failing to support natural testosterone production, and if testosterone replacement therapy is needed.
Common Medications used for HPTA Restart
Physicians will typically use one or more of these medications in a personalized regimen that considers the patients previous hormone use, current condition, and other factors assessed during the appointment. This list is not all-inclusive, since there are similar medications sometimes used by specialists depending on their experience with the drug and their goals for the patient.
- Human Chorionic Gonadotropin (HCG)
- Clomiphene citrate capsules or tablets
- Tamoxifen citrate capsules or tablets
- Toremifene citrate tablets
- Low dose anastrozole
- PDE5 inhibitor like tadalafil or sildenafil to treat erectile dysfunction
When to Start Therapy
When discontinuing a long-acting injectable ester, such as cypionate or enanthate, therapy to stop TRT is usually initiated roughly five days after the last injection, as the hormone levels start to fall.
For faster-acting dosage forms like topical creams and suspensions, HPTA treatment should typically be initiated one day after administering the last dose.
Patients discontinuing hormone pellet therapies need to wait at least two months after insertion before hormone levels begin to fall.
Many progressive testosterone physicians prescribe HCG for men to take during testosterone replacement therapy to help maintain testicular volume and fertility. Using HCG during hormone supplementation can help the HPTA recover faster after hormones are discontinued.
Blood Work for Discontinuing TRT
Laboratory tests are used to determine the effectiveness of the treatment, because they allow the physician to look at hormone levels. Certain hormones should be responding to treatment, and if they are not responding, adjustments can be made to the protocol.
Some of the hormone and metabolic markers tested include:
- Testosterone free and total
- Estradiol (sensitive)
- Luteinizing hormone (LH)
- CBC
- CMP
- Lipids
Results-Driven Protocols for Stopping TRT
Patient success is measured by how they respond to treatment. The goal is to restore endogenous (natural) hormone production to adequate levels and alleviate any negative symptoms that affect quality of life.
In rare cases, someone may not be able to produce hormones on their own. This is called primary hypogonadism and results from the testicles’ inability to respond to LH (or HCG) stimulation. This in turn results in low testosterone production. Patients diagnosed with primary hypogonadism can benefit from testosterone replacement therapy managed by an experienced physician.
The result is relief of symptoms and improvement of metabolic and endocrine health.
Expertly Guided HPTA Restart with Defy Medical
If you want to discontinue TRT safely with limited side effects, Defy Medical can help. We have protocols to assist patients in restarting their HPTA axis.
If you experience low Testosterone, this process won’t stop your low T symptoms from returning once you resume your natural production levels. But it can help you avoid avoid hormone withdrawal symptoms for a more comfortable transition.
Ready to learn more?
* denotes a required field.