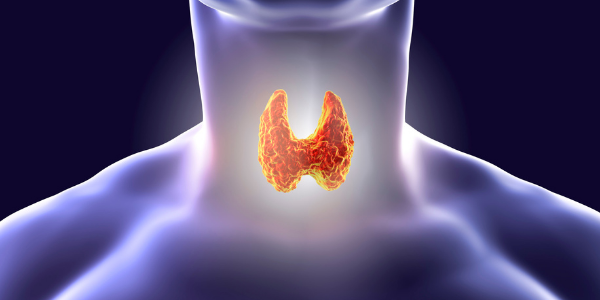
Balance thyroid hormones with Defy Medical.
Thyroid Disease Therapy


Thyroid disease is often underdiagnosed and undertreated.
An estimated 20 million people in the U.S. have thyroid disease – but as many as 60% of people with a thyroid condition don’t even realize it’s the cause of their symptoms.
Bring your body back into balance to feel better and have more energy. Defy Medical specializes in thyroid treatments via telemedicine.
Get Started

Hypothyroidism and Hyperthyroidism Symptoms
- Fatigue
- Sensitivity to cold
- Dry, thinning hair and skin
- Insomnia
- Muscle weakness
- Unexplained weight changes
- Irregular heartbeat
- Puffiness and swelling
- Irritability and anxiety
Blood tests show your thyroid hormone levels.
Diagnosing Thyroid Conditions
To develop an effective treatment plan, we need to know exactly what’s going on in your body. Defy Medical offers access to affordable and comprehensive blood testing, so we can understand the complete picture of your thyroid health. Then we create a treatment plan targeted to your needs.
Testing also helps screen for other potential conditions which can impact thyroid function.
Hypothyroidism and Hyperthyroidism Treatment Options
Treating thyroid disease can help you find relief from your symptoms, so you feel better.
Hormone restoration is usually the best treatment for hypothyroidism (when your body doesn’t produce enough thyroid hormone).
Defy Medical offers access to high-quality treatment options that can help increase your T3 and T4 levels and ease your thyroid disease symptoms.
When patients optimize their thyroid hormones, they almost always report symptom relief.
In addition to prescription medication, nutritional supplements can support thyroid health and overall wellness. Defy Medical offers access to quality and affordable supplements.
In your consultation, a knowledgeable provider will walk you through your options.
Typically, supplements alone aren’t enough to treat thyroid conditions. But they can part of a comprehensive plan that helps you feel your best.




Thyroid hormones are crucial to how your body functions.
What is Thyroid Disease?
The thyroid produces hormones T3 (triiodothyronine) and T4 (thyroxine). Together, T3 and T4 help regulate your entire system.
Thyroid disease occurs when your thyroid produces too much or too little of these hormones. Your body can’t function properly, leading to noticeable symptoms.
Thyroid disease can be caused by autoimmune conditions, swelling, iodine deficiency or excess, genetic factors, and endocrine tumors.
Defy Medical: Your Integrative Medicine Experts
For more than a decade, Defy Medical has offered integrative treatments in-office and via telemedicine. Led by Medical Director Dr. Justin Saya, our experienced care team has guided thousands of patients to living happier, healthier lives – and we’re ready to help you.
With Defy Medical, you access:

Expert Care
Our experienced care team treats patients using the latest advancements in integrative therapies.

Convenient Telemedicine
Save time consulting with experienced providers via telemedicine and ordering medications (if prescribed) online.

No Subscriptions or Contracts
You control your schedule and cost decisions, and only pay for what you need.

Extended Consults
You can book a consult to get one-on-one guidance and discuss any concerns.

Individualized Care Plans
We go deeper to get to the root causes and create a treatment plan as unique as you are.

Regular Follow-Up
Work with our providers over time to find the treatment that fits you the best.
A Wide Range of Treatment Options
We offer access to a variety of compounded and name brand medication options.
A Variety of Health Services
A variety of health services. We also offer Hormone Replacement Therapy, nutritional supplementation, Primary Care, and more.

More Services
You Might Also Be Interested In:

Fat Loss
Losing weight can be complicated. Our fat loss program gets to the root cause of your weight gain and provides the tools to help you reach your fat loss goals.

Vitamins & Supplements
Optimize your performance and improve your quality of life with IV therapy in Tampa, FL. Deliver nutrients to your bloodstream for maximum absorption.